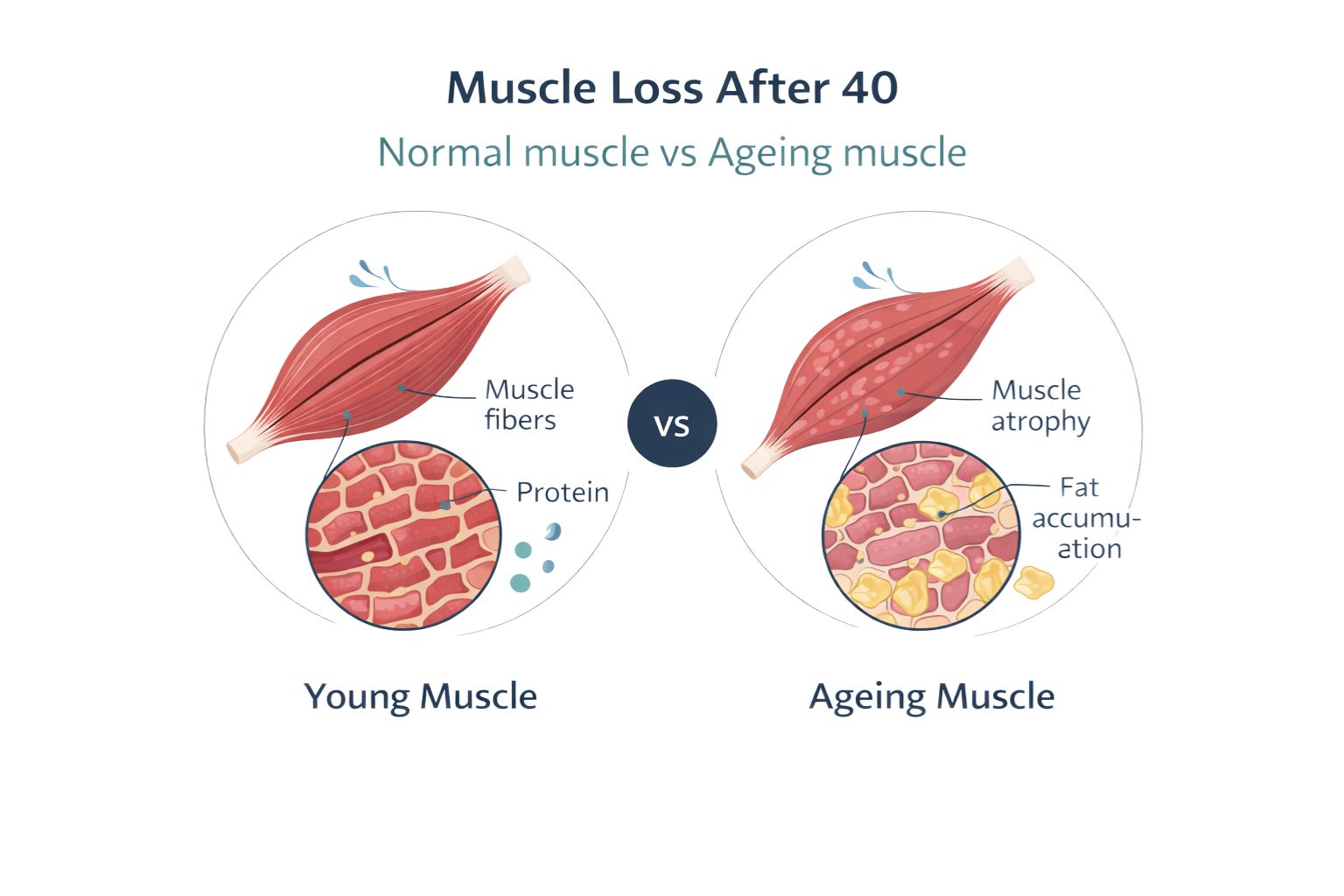
As the human body progresses beyond the fourth decade, biological shifts occur that influence physical capability and body composition. One of the most significant yet frequently overlooked transitions is the gradual decline of skeletal muscle mass. While a degree of change is expected as part of the natural aging process, an accelerated or excessive loss is categorized medically as sarcopenia.
Sarcopenia is defined as an age-related, progressive, and generalized skeletal muscle disorder involving the accelerated loss of muscle mass and function. While this condition typically becomes most visible after age 60, the physiological foundations are often established much earlier, starting in the 40s. Understanding the distinction between natural biological maturation and pathological muscle loss is essential for maintaining long-term mobility and independence.
The following guide serves to translate clinical research into practical observations, helping individuals and caregivers identify the primary sarcopenia symptoms and determine the appropriate evidence-based interventions.
The Biological Context of Muscle Loss After 40
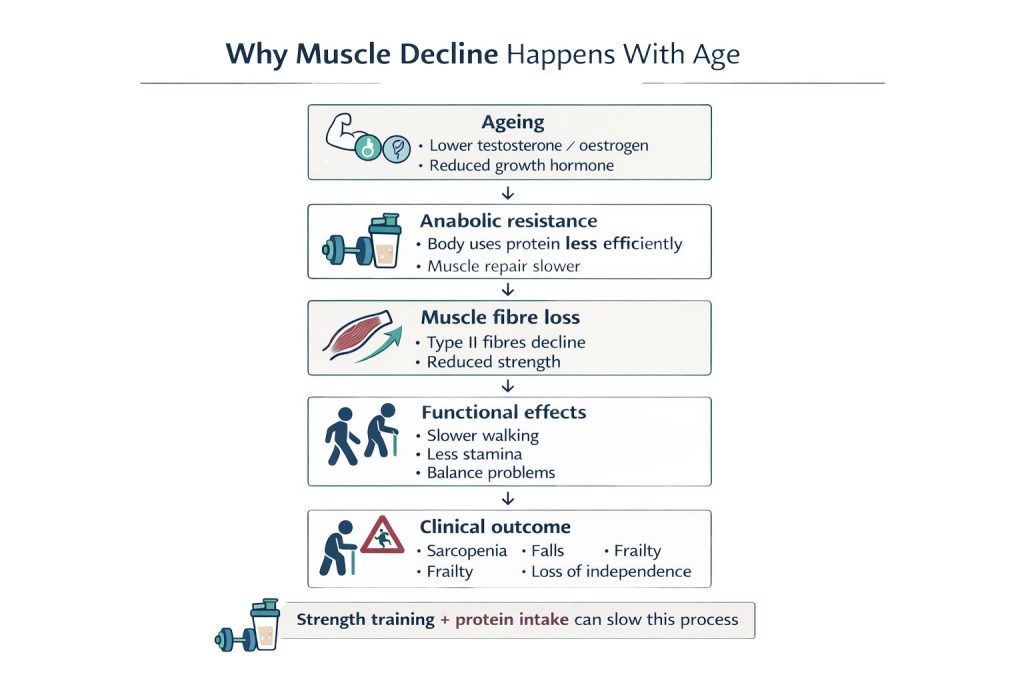
To understand sarcopenia, one must first recognize the relationship between aging and muscle protein synthesis. In younger adults, the body efficiently balances the breakdown of muscle tissue with the creation of new fibers. However, after age 40, this balance begins to shift. Research indicates that most adults lose approximately 3% to 8% of their muscle mass per decade after age 30, a rate that increases significantly once an individual reaches age 60.
This decline is not merely a matter of aesthetics; it represents a fundamental change in metabolic health. Muscles serve as the body’s primary reservoir for amino acids and play a critical role in glucose regulation. Therefore, muscle loss after 40 can have a cascading effect on overall systemic health, increasing the risk of type 2 diabetes and cardiovascular complications.
5 Ways to Spot Sarcopenia Symptoms
Identifying sarcopenia in its early stages requires a structured observation of physical performance and daily habits. The platform emphasizes the importance of objective monitoring to separate "feeling tired" from clinical muscle degradation.
1. Significant Muscle Weakness
The primary indicator of sarcopenia is a noticeable reduction in strength. This often manifests during tasks that were previously effortless. For example, an individual might find that they struggle to lift objects they managed with ease only a year or two prior. In clinical settings, this is often measured through handgrip strength, which serves as a reliable proxy for overall body strength and a predictor of future disability.
2. Reduced Stamina and Persistent Fatigue
Sarcopenia affects the quality of muscle fibers, not just the quantity. As the proportion of type II (fast-twitch) fibers decreases, the body’s ability to sustain physical exertion diminishes. If an individual experiences a loss of staying power during routine physical activity, such as feeling winded after a short walk or needing to rest more frequently during household chores, it may indicate that the underlying muscle architecture is no longer supporting the body's aerobic demands efficiently.
3. Difficulty with Everyday Movements
One of the most practical ways to assess muscle health is to observe "activities of daily living" (ADLs). Clinical research highlights several red flags:
- Difficulty climbing stairs: Requiring the use of a handrail for balance or strength.
- Rising from a chair: Needing to push off the armrests with the hands to stand up.
- Manual dexterity: Finding it increasingly difficult to open jars or carry heavy grocery bags.
When these movements transition from being automatic to requiring conscious effort, it is often a sign of declining functional mass.
4. Slower Walking Speed and Balance Issues
There is a high correlation between muscle mass and gait speed. A reduction in the strength of the lower extremities, specifically the quadriceps and glutes, directly impacts stride length and stability. This leads to a slower walking pace and, more critically, impaired balance. Because muscles act as the body’s stabilization system, their loss increases the risk of falls and subsequent fractures, a leading cause of hospitalization in older populations.
5. Visibly Shrinking Muscles (Atrophy)
While subcutaneous fat can sometimes mask muscle loss, visible atrophy is a clear clinical sign. This is most often observed in the limbs. If the arms or legs appear noticeably thinner or "looser" than in previous years, or if clothing fits differently despite no change in overall body weight, it suggests a shift in body composition where muscle is being replaced by adipose tissue or simply lost entirely.

Is This Normal or Is It Sarcopenia?
A common challenge for adults over 40 is distinguishing between the natural "slowing down" of age and a condition that requires medical attention. The platform provides a dedicated resource to help individuals navigate this distinction: is this normal.
Generally, natural aging involves a subtle decline that does not prevent an individual from performing their usual activities. Sarcopenia, however, is characterized by a loss of function that limits independence. If the symptoms listed above are interfering with your quality of life or increasing your fear of falling, the condition has likely moved beyond the scope of "normal aging" and requires a proactive management plan.
What to Do Next: Evidence-Based Interventions
The diagnosis of sarcopenia is not a permanent sentence of decline. Because the musculoskeletal system remains plastic, meaning it can adapt and grow even in older age, specific lifestyle interventions can significantly mitigate or even reverse muscle loss after 40.
Nutritional Optimization: The Protein Requirement
The aging body becomes less efficient at processing protein, a phenomenon known as "anabolic resistance." Consequently, adults over 40 require a higher proportion of dietary protein to stimulate muscle protein synthesis compared to younger individuals.
Current research suggests that for those at risk of sarcopenia, a protein intake of 1.2 to 1.5 grams per kilogram of body weight is often necessary. Distributing this protein evenly across all meals, rather than consuming it mostly at dinner, ensures the body has a consistent supply of amino acids throughout the day to repair and build tissue.
Resistance and Strength Training
Physical activity is the most potent tool available to combat sarcopenia symptoms. Specifically, resistance training (weight lifting, resistance bands, or bodyweight exercises) is the gold standard for intervention. Resistance training creates microscopic tears in the muscle fibers, which, when paired with adequate nutrition, signal the body to rebuild the tissue stronger and denser.
For those over 40, a structured program focusing on major muscle groups twice a week can yield significant improvements in strength and metabolic health.
Medical Monitoring and Professional Guidance
If you suspect that you or someone you care for is exhibiting signs of sarcopenia, the next step is professional consultation. A healthcare provider can perform objective tests, such as:
- SARC-F Questionnaire: A screening tool that assesses strength, walking assistance, rising from a chair, stair climbing, and falls.
- Gait Speed Test: Measuring the time it takes to walk a set distance.
- DXA Scans: Used to provide a precise measurement of lean body mass.
For more information on navigating the healthcare system and understanding clinical terminology, visit our guides section.
Conclusion: Taking a Pedagogical Approach to Aging
Addressing muscle loss after 40 requires a shift from passive observation to active management. By recognizing the specific symptoms of sarcopenia, weakness, fatigue, difficulty with daily tasks, balance issues, and visible atrophy, individuals can make informed decisions about their health long before mobility is compromised.
Understanding Ageing is committed to providing the educational resources necessary to separate myth from medical reality. To learn more about our mission and our commitment to evidence-based health education, please visit about us. By applying the principles of targeted nutrition and resistance training, it is possible to maintain a high level of physical function and ensure that the later decades of life are characterized by strength and independence.