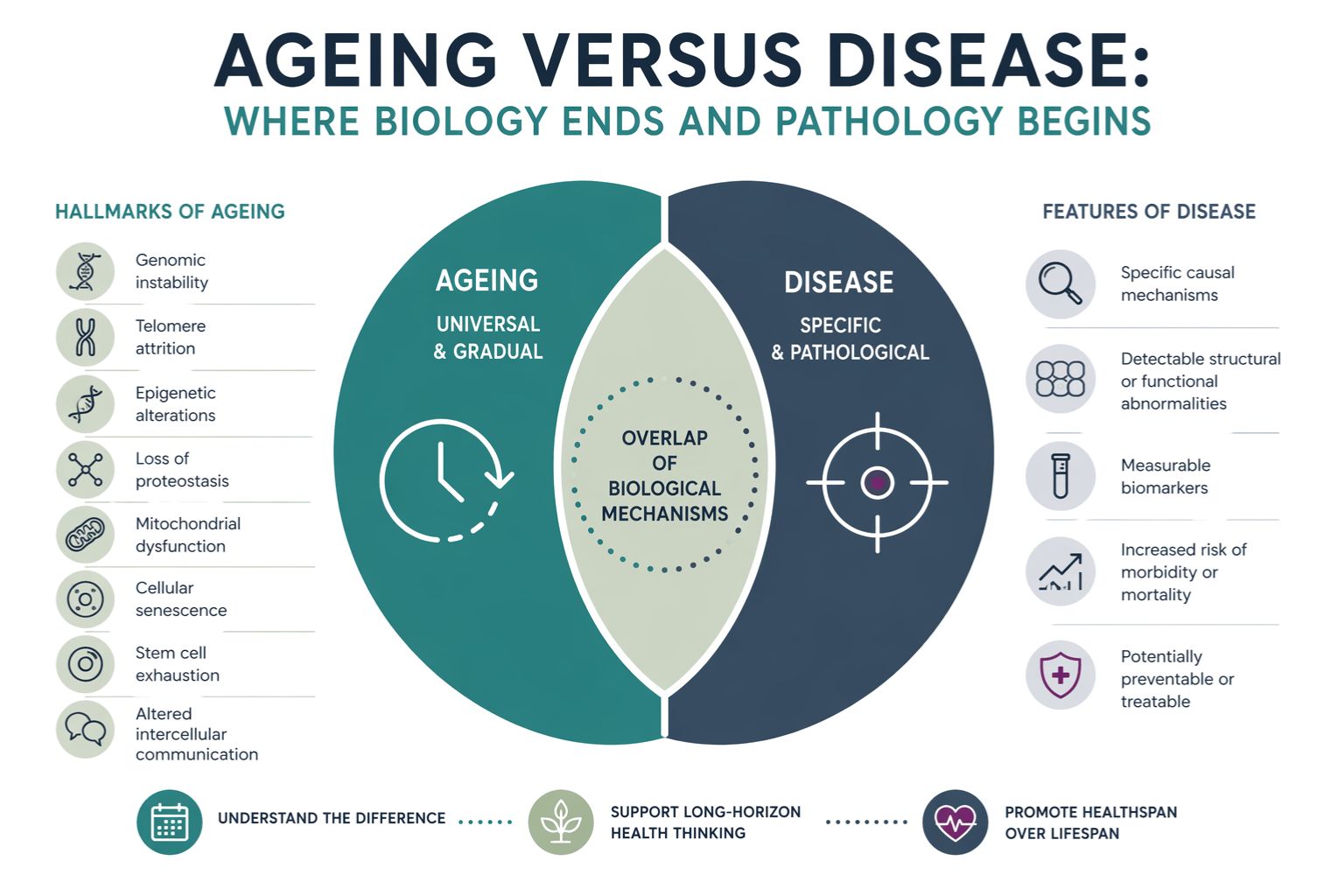
Ageing is an inevitable part of life, bringing with it a myriad of changes that can affect our physical, cognitive, and emotional well-being. As individuals transition into their later years, they often encounter various symptoms that may lead to confusion, concern, or even fear. Understanding whether these symptoms are a normal part of ageing or indicative of a more serious health issue is crucial. This article aims to provide a structured framework for evaluating symptoms associated with ageing, emphasising the significance of clinical reasoning and the importance of cultivating long-term trust with healthcare providers.
Understanding Ageing
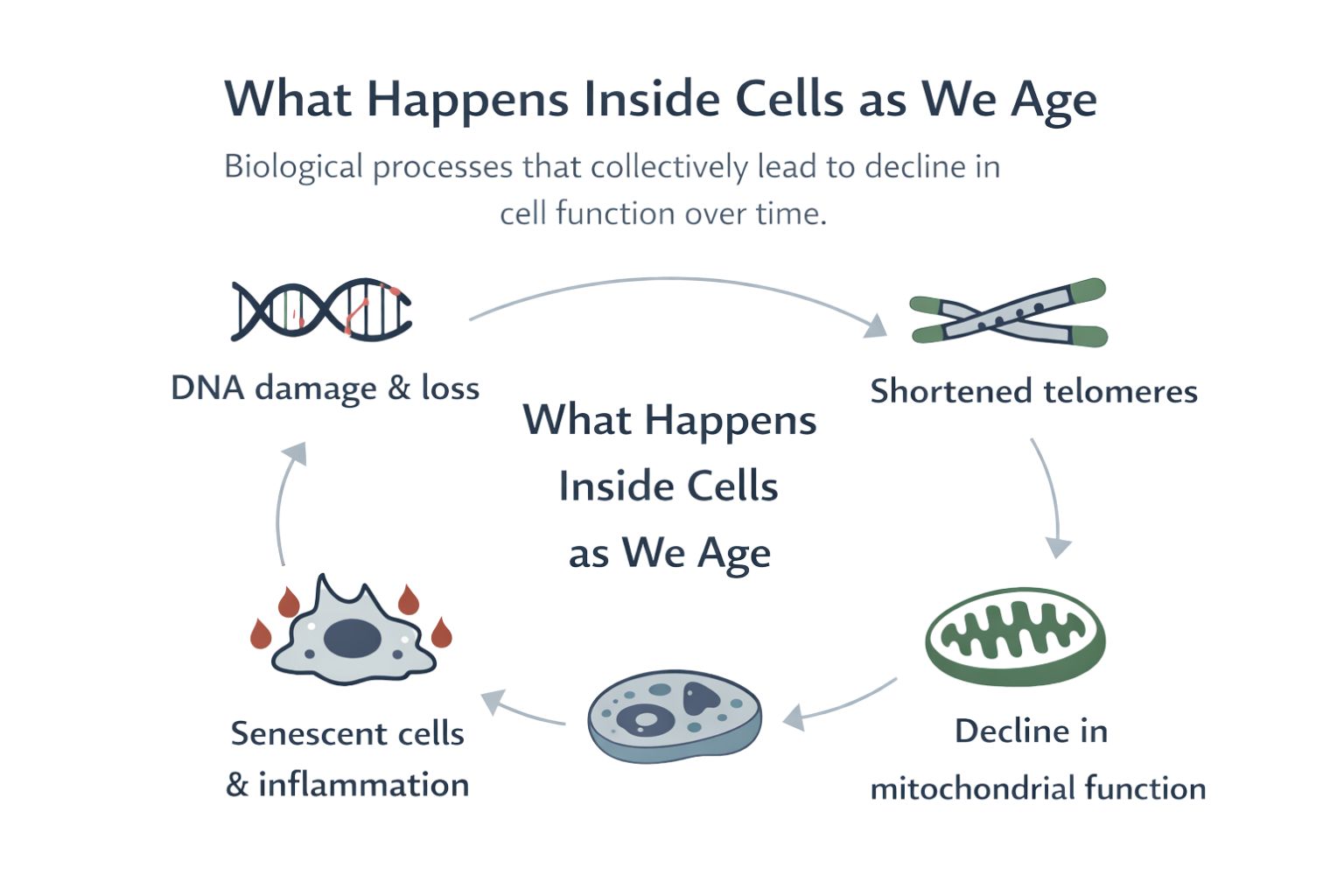
As we age, our bodies undergo a series of physiological changes that can impact our overall health. Muscle mass typically declines, leading to decreased strength and increased susceptibility to falls and fractures. Bone density also diminishes, particularly in post-menopausal women, making bones more fragile and prone to breaks. Additionally, skin loses collagen and elasticity, resulting in wrinkles and dryness. While these changes can manifest as symptoms, they are often a normal part of the ageing process.
Cognitive decline can vary widely among older adults. Occasional forgetfulness is common, but persistent memory loss may indicate conditions such as mild cognitive impairment or Alzheimer’s disease. Emotional health is equally important, as feelings of anxiety and depression can arise from various factors, including loss, loneliness, or chronic pain. Recognising these psychological changes is essential for evaluating symptoms holistically.
Social dynamics also play a crucial role in health as we age. Many older adults experience social isolation due to retirement or the loss of friends and family members. This loneliness can exacerbate physical and emotional health issues. Maintaining strong relationships with family, friends, and community members can greatly enhance emotional well-being and improve health outcomes.
Common Symptoms in Ageing
As individuals age, they may experience a range of physical, cognitive, and emotional symptoms. Among the most common physical symptoms are joint pain, fatigue, and skin changes. Conditions like osteoarthritis are prevalent and can impede mobility. It is essential to assess whether pain is chronic or temporary, as this can guide treatment options. Persistent fatigue, on the other hand, can stem from various sources, including sleep disorders, nutritional deficiencies, or underlying medical conditions.
Cognitive symptoms can also vary widely. While occasional memory lapses are normal, significant memory loss affecting daily life should be evaluated by a healthcare professional. Attention issues, such as difficulty concentrating, may be linked to stress, medication side effects, or early cognitive decline. Emotional symptoms, including anxiety and depression, often go unrecognised. These conditions may manifest as sadness, withdrawal from social activities, or changes in appetite and sleep. Recognising these symptoms early can lead to effective interventions and better mental health outcomes.
Evaluating Symptoms: The Clinical Reasoning Framework
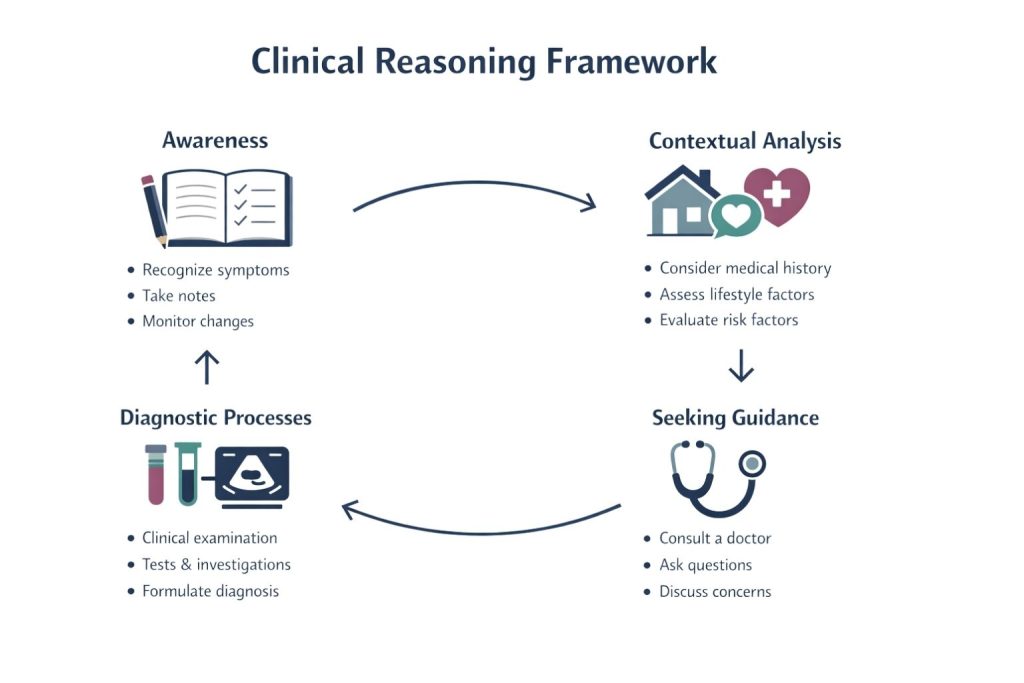
Evaluating symptoms effectively requires a structured approach. The first step is symptom awareness. Being aware of and acknowledging symptoms is crucial for prompt evaluation. Keeping a symptom diary can be a useful tool for tracking changes over time, helping individuals provide valuable information to healthcare providers.
Next, contextual analysis is essential. Evaluating symptoms in the broader context of overall health involves assessing lifestyle factors such as diet, exercise, and sleep habits. It is also important to consider how existing chronic conditions may interact with new symptoms, as this holistic view can help determine whether symptoms are typical for an individual’s age and health status.
Seeking professional guidance is critical for proper evaluation. Consulting healthcare providers allows individuals to gain insights into their symptoms and potential treatment options. Clear communication about symptoms, including their duration and impact on daily life, can lead to more effective diagnosis and treatment. Preparing questions in advance can also help ensure that all concerns are addressed during appointments.
Understanding diagnostic processes can alleviate anxiety. Familiarising oneself with common tests and procedures can demystify the healthcare process. Knowing what to expect can ease the experience of seeking medical care, making it less daunting.
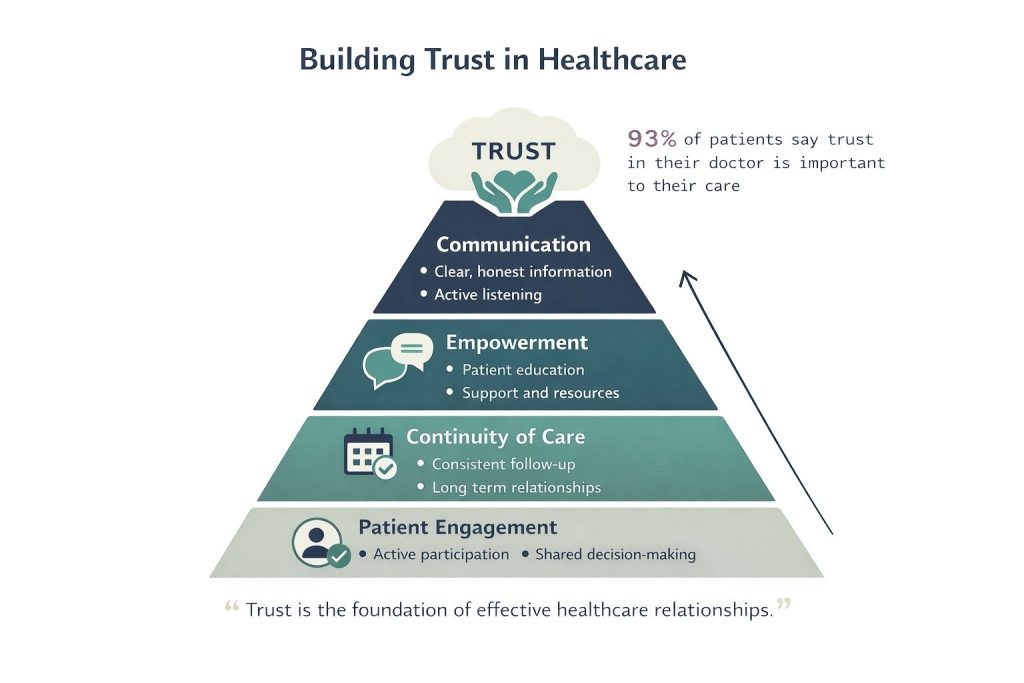
Building Long-Term Trust with Healthcare Providers
Establishing a strong relationship with healthcare providers is vital for effective healthcare. A solid patient-provider relationship is built on trust and open communication. Regularly discussing health concerns and treatment options fosters a collaborative relationship, enhancing trust and understanding.
Empowering patients to take an active role in their health decisions is equally important. Encouraging individuals to ask questions, voice concerns, and advocate for their needs can lead to better health outcomes and satisfaction. Patients should feel confident in their ability to seek clarification about their health and treatment plans.
Continuity of care also plays a vital role in building trust. Having a consistent healthcare team allows providers to understand individual health histories and preferences, leading to more personalised care. Regular check-ups and follow-up appointments help monitor ongoing issues and adjust treatments as necessary.
The Role of Technology in Monitoring Symptoms
In today’s digital age, technology can play a significant role in health monitoring. Wearable devices and health apps can help track symptoms, vital signs, and activity levels, providing valuable data for both patients and healthcare providers. This data can enhance the accuracy of evaluations and treatment plans.
Telehealth services offer unique advantages, especially for individuals with mobility issues or those living in remote areas. These services provide essential access to healthcare, facilitating ongoing communication and monitoring. Virtual appointments can help ensure that symptoms are addressed promptly and effectively.
When Symptoms Are Cause for Concern
Certain symptoms should prompt immediate medical attention. Sudden changes, such as severe headaches, vision changes, or unexplained weight loss, can indicate serious health conditions and should not be ignored. Additionally, recognising emergency signs, such as symptoms of a stroke or heart attack, is crucial for timely intervention.
It is essential to differentiate between normal ageing and potential health issues. If a symptom feels unusual or concerning, seeking professional advice is vital. Trusting one’s instincts and advocating for personal health is an important aspect of managing well-being as we age.
Conclusion
Navigating the complexities of ageing requires a proactive approach to health. By understanding the ageing process, recognising symptoms, and following a structured framework for evaluation, individuals can make informed decisions regarding their health. Building long-term trust with healthcare providers fosters a supportive environment where patients feel empowered to take charge of their well-being. Embracing the journey of ageing with knowledge, awareness, and support can lead to a healthier, more fulfilling life.